
38-Year-Old Female with Preeclampsia
Ms. Johansen, 38, is 26 weeks pregnant with her first child. She was diagnosed with preeclampsia (see p. 1114) three weeks ago. Antihypertensive drugs (p. 724) and daily home care monitoring were initiated. However, her blood pressure is continuing to rise and is now 162/108 mm Hg. She complains of a constant headache, exhibits edema, and her urinalysis is positive for protein.
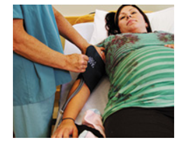
Her doctor has her admitted and orders further blood tests to assess Ms. Johansen's platelet level and liver function. "We may have to deliver because that’s the only cure for preeclampsia." she says to you during your clinical rotation in obstetrics. “But if we do, then the baby will have problems. It’s a tough decision because we have to balance both the mother's and the baby’s health.”
4. What roles does cortisol play in a developing fetus and how would an injection of cortisol help a premature infant?
Want to see the full answer?
Check out a sample textbook solution
Chapter 28 Solutions
HUMAN ANATOMY+PHYSIOLOGY-ACCESS(IAC)
- How is a protein destined for the Endoplasmic Reticulum (ER), imported into the ER? Be concise.arrow_forwardFind out about the organisations and the movements aimed at the conservation of our natural resources. Eg Chipko movement and Greenpeace. Make a project report on such an organisation.arrow_forwardWhat are biofertilizers and mention the significancearrow_forward
- PCBs and River Otters: Otters in Washington State’s Green-Duwamish River have high levels of polychlorinated biphenyls (PCBs) in their livers. PCBs can bind to the estrogen receptors in animals and disrupt the endocrine system of these otters. The PCBs seem to increase the estrogen to androgen ratio, skewing the ratio toward too much estrogen. How would increased estrogen affect the river otter population? Based on your reading of the materials in this unit, what factors can affect fertility in humans? Explain how each of the factors affecting human fertility that you described can disrupt the human endocrine system to affect reproduction.arrow_forwardOther than oil and alcohol, are there other liquids you could compare to water (that are liquid at room temperature)? How is water unique compared to these other liquids? What follow-up experiment would you like to do, and how would you relate it to your life?arrow_forwardSelection of Traits What adaptations do scavengers have for locating and feeding on prey? What adaptations do predators have for capturing and consuming prey?arrow_forward
- Competition Between Species What natural processes limit populations from growing too large? What are some resources organisms can compete over in their natural habitat?arrow_forwardSpecies Interactions Explain how predators, prey and scavengers interact. Explain whether predators and scavengers are necessary or beneficial for an ecosystem.arrow_forwardmagine that you are conducting research on fruit type and seed dispersal. You submitted a paper to a peer-reviewed journal that addresses the factors that impact fruit type and seed dispersal mechanisms in plants of Central America. The editor of the journal communicates that your paper may be published if you make ‘minor revisions’ to the document. Describe two characteristics that you would expect in seeds that are dispersed by the wind. Contrast this with what you would expect for seeds that are gathered, buried or eaten by animals, and explain why they are different. (Editor’s note: Providing this information in your discussion will help readers to consider the significance of the research).arrow_forward
- Basic Clinical Lab Competencies for Respiratory C...NursingISBN:9781285244662Author:WhitePublisher:Cengage
- Understanding Health Insurance: A Guide to Billin...Health & NutritionISBN:9781337679480Author:GREENPublisher:Cengage
 Microbiology for Surgical Technologists (MindTap ...BiologyISBN:9781111306663Author:Margaret Rodriguez, Paul PricePublisher:Cengage Learning
Microbiology for Surgical Technologists (MindTap ...BiologyISBN:9781111306663Author:Margaret Rodriguez, Paul PricePublisher:Cengage Learning





